CALEC surgery represents a groundbreaking advancement in the treatment of eye damage, particularly for individuals suffering from corneal injuries previously deemed untreatable. This innovative procedure, which stands for cultivated autologous limbal epithelial cells, has shown remarkable promise in restoring the cornea’s surface using stem cell therapy. During a clinical trial led by experts at Mass Eye and Ear, it was revealed that CALEC successfully rehabilitated the corneas of 14 participants, highlighting a success rate exceeding 90% over 18 months. By harvesting limbal epithelial cells from a healthy eye, CALEC harnesses the body’s regenerative capabilities to repair severe eye damage, offering new hope for patients enduring chronic pain and vision issues. As researchers continue to explore the potential of eye damage treatment, CALEC surgery embodies the forefront of corneal restoration techniques.
The introduction of cultivated autologous limbal epithelial cells, commonly referred to as CALEC, ushers in a transformative option for individuals with severe ocular injuries. This advanced surgical technique focuses on extracting stem cells from a donor eye, subsequently using them to create a graft that can restore the corneal surface. With the growing body of evidence supporting the efficacy of stem cell therapy for eye restoration, the clinical trials associated with CALEC stand as a testament to innovation in eye care. As researchers and health professionals aim to enhance the prospects of patients at risk of corneal complications, the potential for improved outcomes in eye health is on the horizon. By prioritizing limbal epithelial cell regeneration, CALEC surgery paves the way for a brighter future in ocular medicine.
What is CALEC Surgery?
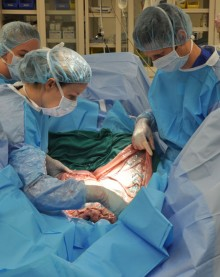
Cultivated Autologous Limbal Epithelial Cells (CALEC) surgery is a groundbreaking procedure aiming to repair the corneal surface in patients suffering from severe eye damage, often as a result of trauma or disease. This innovative surgery involves extracting healthy limbal epithelial cells from the patient’s unaffected eye, expanding these cells in a controlled environment, and then grafting them onto the damaged cornea. The process addresses limbal stem cell deficiency, a condition that can leave patients unable to undergo traditional corneal transplants, thus making CALEC an essential treatment for restoring vision and alleviating persistent discomfort.
The development of CALEC surgery emerged from extensive research and trials, demonstrating its effectiveness and safety in clinical settings. Ula Jurkunas, a leading researcher in this field, highlights that the initial trial of CALEC surgery yielded more than 90% success in restoring corneal surfaces after 18 months. This significant advancement opens new avenues for patients with extensive corneal injuries previously considered untreatable, marking a monumental shift in eye damage treatment.
The Role of Stem Cell Therapy in Eye Restoration
Stem cell therapy has revolutionized the landscape of regenerative medicine, particularly in eye care. By harnessing the power of stem cells, medical professionals can develop advanced treatments like CALEC surgery to rejuvenate damaged ocular surfaces. Stem cells possess the unique ability to proliferate and differentiate into various cell types, making them ideal candidates for repairing injured tissues. In the context of eye damage treatment, the application of stem cells from healthy donor tissue promotes regeneration where natural healing processes have faltered.
In recent clinical trials, stem cell therapy has successfully restored the integrity of the corneal surface in numerous patients. The ability to employ cultivated stem cells to rehabilitate the ocular surface has demonstrated potential not only for healing but for significantly improving visual acuity over time. As research continues to evolve, the integration of stem cell therapy offers newfound hope for individuals seeking effective solutions for blinding corneal injuries.
Understanding Limbal Epithelial Cells
Limbal epithelial cells play a crucial role in maintaining the health and transparency of the corneal surface. These specialized cells are located at the limbus, the border between the cornea and the sclera. They serve as the source of regenerative cells for the cornea, facilitating continuous repair and maintenance. In cases of injury or disease, depletion of limbal epithelial cells can lead to limbal stem cell deficiency, resulting in chronic pain and vision loss. Therefore, understanding and preserving the function of these cells is integral to the success of treatments like CALEC surgery.
Research has revealed that conditions such as chemical burns, infections, or even congenital issues can drastically impact the population and function of limbal epithelial cells. As such, therapies aimed at replenishing these cells, such as those utilized in CALEC surgery, are of utmost importance. By restoring these vital cells, patients can achieve not only relief from debilitating symptoms but also a significant improvement in their overall quality of life.
Clinical Trials and Innovations in Eye Care
Clinical trials are fundamental in evaluating the effectiveness and safety of new medical treatments, including those targeting eye conditions. The pioneering CALEC surgery, for instance, underwent rigorous clinical trials at Mass Eye and Ear to ensure comprehensive assessment before potential wider adoption. These trials not only gauge how well the treatment works but also monitor the long-term effects and any adverse reactions, emphasizing patient safety and treatment efficacy.
In the case of CALEC, the clinical trial results showed promising outcomes, with significant percentages of patients experiencing full and partial restoration of corneal surfaces. This data is crucial for driving future research and innovations in the field of ophthalmology, as well as for pursuing avenues towards FDA approval. Comprehensive clinical studies like these set the groundwork for transforming experimental therapies into widely accessible treatments for eye damage.
Future Directions for Limbal Stem Cell Therapy
The future of limbal stem cell therapy, particularly with techniques like CALEC, looks promising. Research is ongoing to refine and enhance the methodology for better success rates and broader applicability. Encouragingly, there are discussions around developing allogeneic manufacturing processes that would allow stem cells from healthy donors to be used for transplantation in patients with bilateral corneal injuries, thereby expanding access to this groundbreaking treatment.
Furthermore, advancing technologies and collaborative efforts among researchers and clinicians will be vital in solidifying the role of stem cell therapy within ocular medicine. Future trials are expected to encompass larger populations, diverse demographic groups, and more extensive follow-ups to gather robust data. Such efforts will ultimately help prepare the groundwork for the approval and implementation of CALEC and similar therapies in routine clinical practice.
Success Rates of CALEC Surgery
The success rates of CALEC surgery from recent clinical trials indicate a bright future for patients facing severe corneal damage. In initial trials, it was found that at three months post-surgery, around 50% of participants experienced full corneal restoration, with this figure increasing to approximately 79% and 77% at the 12- and 18-month marks, respectively. These figures reflect not only the procedure’s immediate benefits but also its lasting impact on patients’ vision and comfort.
Assessing the success of CALEC surgery offers significant insights into the treatment of corneal injuries. Moreover, the observed improvements in visual acuity among participants further demonstrate the substantial advantages afforded by this pioneering stem cell therapy. As this research continues to evolve, it’s clear that high success rates bolster the case for broader implementation in clinical settings, potentially reshaping treatment protocols for eye damage.
Safety Profile of CALEC Surgery
The safety profile of CALEC surgery is particularly important given the delicate nature of eye procedures. Initial clinical trials have reported a high safety rate, with no significant complications occurring in the majority of cases. Notably, any adverse events tended to be minor and manageable, indicating that the benefits of the surgery largely outweigh the risks associated with the procedure.
Moreover, the absence of serious adverse events associated with either the donor or recipient eyes underscores the careful planning and execution of the surgical process. Continuous monitoring of treated patients will remain essential in affirming the safety of CALEC surgery as it progresses towards broader clinical availability. As ongoing studies yield further insights, patient safety and satisfaction can be prioritized in the evolution of ocular therapies.
The Impact of CALEC on Patient Quality of Life
The advent of CALEC surgery not only signifies a shift in clinical ophthalmology but also heralds a profound impact on the quality of life for patients suffering from corneal damage. Many patients with limbal stem cell deficiency experience debilitating symptoms, including significant pain and visual impairment. The successful restoration of their corneal surface through CALEC surgery translates into enhanced vision and reduced discomfort, which can be life-changing.
Furthermore, as patients reclaim their vision through innovative treatments such as CALEC, there are broader implications for their mental and emotional well-being. Improved sight can lead to a resurgence of independence, allowing individuals to engage in everyday activities and regain a sense of normalcy in their lives. The positive ripple effects of such a transformative treatment underscore the importance of continued research and investment in stem cell therapies for eye care.
Collaborative Research in Ocular Regeneration
The development of therapies like CALEC surgery exemplifies the power of collaborative research in the field of ocular regeneration. Efforts among institutions such as Mass Eye and Ear, Dana-Farber Cancer Institute, and Boston Children’s Hospital have paved the way for significant advances. Such collaborative frameworks enable the confluence of expertise across diverse fields—ranging from clinical trials to cell manufacturing—strengthening the overall research output and application.
Future success in advancing ocular treatments will greatly depend on continued partnerships and interdisciplinary approaches. As researchers work together to share findings and techniques, the journey from concept to clinical application can accelerate. This communal effort is essential for evolving innovative treatments, ensuring they reach the patients who need them most, and fulfilling the promise of regenerative medicine in ophthalmology.
Frequently Asked Questions
What is CALEC surgery and how does it help in eye damage treatment?
CALEC surgery, or Cultivated Autologous Limbal Epithelial Cell surgery, is a pioneering procedure that utilizes stem cell therapy to restore corneal surfaces damaged by injuries like chemical burns or trauma. By harvesting limbal epithelial cells from a healthy eye, these cells are cultivated into a graft that can be surgically transplanted to restore vision in the affected eye, making it a promising option for eye damage treatment.
How effective is CALEC surgery in restoring the cornea?
Recent clinical trials have shown that CALEC surgery has over a 90 percent success rate in restoring corneal surfaces. Findings from the trial indicate that 50 percent of participants experienced complete corneal restoration at three months, with rates increasing to 79 and 77 percent at twelve and eighteen months, respectively, demonstrating CALEC’s effectiveness in addressing severe cornea damage.
What role do limbal epithelial cells play in CALEC surgery?
Limbal epithelial cells are crucial for maintaining a healthy corneal surface. In CALEC surgery, these cells are extracted from a patient’s healthy eye, cultivated, and then transplanted to the damaged eye. This process aims to replenish the lost cells due to injury, successfully restoring the cornea and improving vision.
Is CALEC surgery currently available for all patients with corneal damage?
Currently, CALEC surgery is still experimental and not widely available. It is primarily performed within clinical trials at designated research centers like Mass Eye and Ear. Future hopes involve developing an allogeneic process to treat patients with damage to both eyes, increasing access to this innovative eye damage treatment.
What safety profile has been observed in CALEC surgery trials?
CALEC surgery has exhibited a high safety profile, with no severe adverse events reported in the participant’s eyes during trials. There was a minor infection in one participant attributed to contact lens use, but other occurrences were resolved quickly. Overall, the procedure shows promising safety measures for potential broader applications in treating eye damage.
What are the next steps for CALEC surgery after the current clinical trials?
The next steps for CALEC surgery involve conducting larger, multi-center trials with a randomized-control design to gather more extensive data. These studies will aim to confirm efficacy and safety before seeking FDA approval, ultimately leading to a wider availability of this groundbreaking stem cell therapy for corneal restoration.
| Key Point | Details |
|---|---|
| First CALEC surgery performed | Ula Jurkunas performed the first CALEC surgery at Mass Eye and Ear. |
| Key research outcome | CAREC showed over 90% effectiveness in restoring corneal surfaces in clinical trials. |
| Procedure description | Involves harvesting stem cells from a healthy eye to create a graft for transplant. |
| Safety profile | The procedure had no major complications and a high safety profile. |
| Potential for broader application | Future plans aim to establish procedures allowing for treatment in patients with injuries in both eyes. |
| Adverse events | Minimal adverse events were recorded, primarily minor and resolved quickly. |
| Funding and collaboration | The study was funded by the National Eye Institute and involved collaborations with multiple institutions. |
Summary
CALEC surgery represents a groundbreaking advancement in eye treatment, offering new hope to patients suffering from severe corneal injuries. Through the innovative application of stem cell therapy, this pioneering procedure has demonstrated remarkable effectiveness in restoring the cornea’s surface. As research continues and further studies are implemented, CALEC surgery promises to change the landscape of ophthalmology, potentially providing lasting solutions for conditions once deemed untreatable.